Cervical Length and Its Importance in Pregnancy
What is Cervical Length?
Cervical length refers to the length of the cervix—the lower, narrow part of the uterus that opens into the vagina. It is typically measured in millimeters using transvaginal ultrasound, especially during the second trimester of pregnancy.
Normal Cervical Length
In a typical pregnancy, cervical length varies depending on the gestational age:
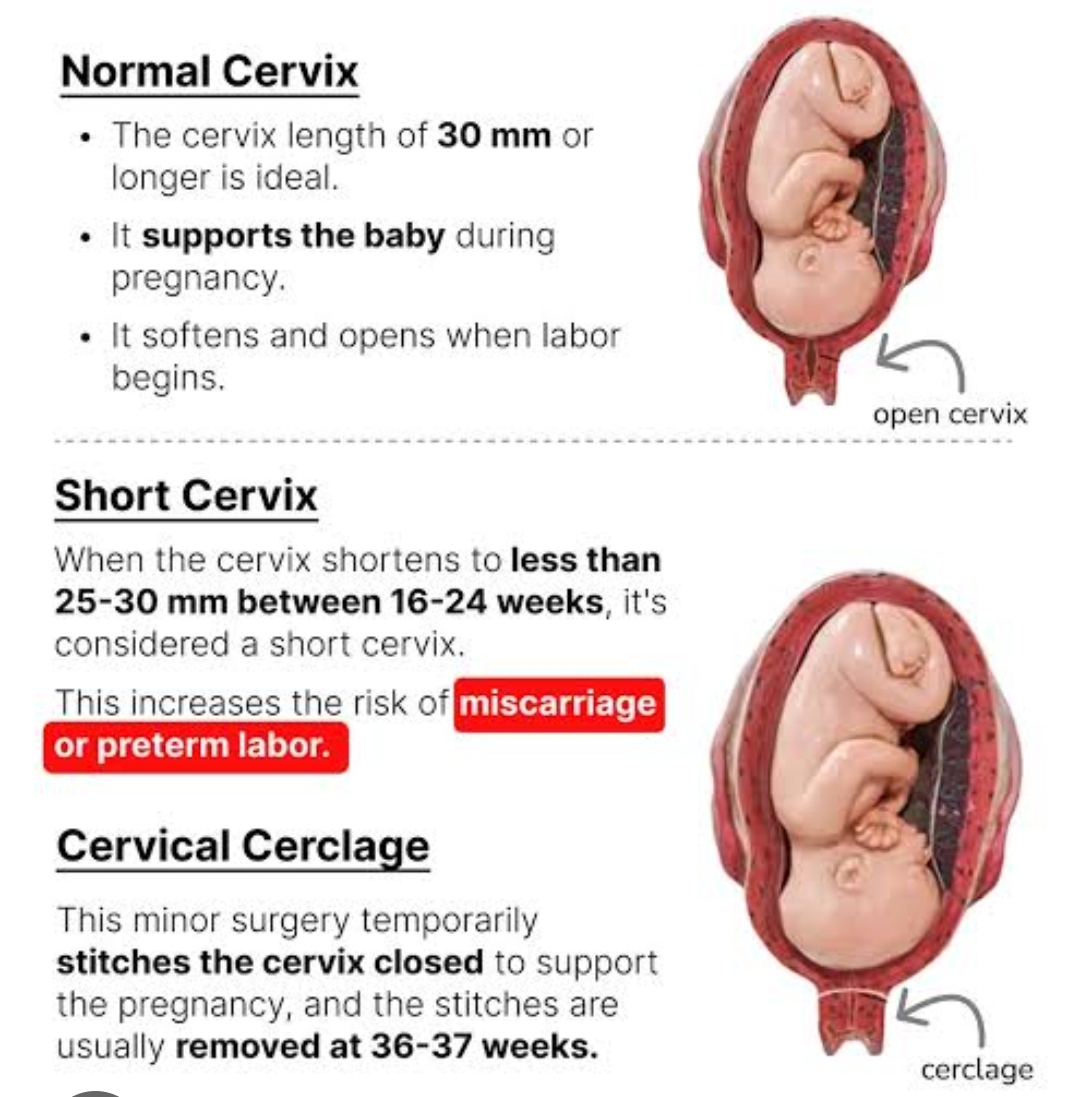
30 mm (3 cm) is considered normal between 16–24 weeks.
A cervical length of 25 mm before 24 weeks is considered short and may increase the risk of preterm birth.
Why Cervical Length Matters
Predicting Preterm Birth
A short cervix (25 mm) is a strong predictor of spontaneous preterm birth, especially in women with a prior history of preterm delivery.
The shorter the cervix, the higher the risk of early labor.
Assessing Risk in High-Risk Pregnancies
Cervical length is especially monitored in:
Women with previous preterm labor.
Those with a history of cervical insufficiency (incompetent cervix).
Women carrying twins or multiples, as they are at higher risk of cervical shortening.
Guiding Treatment
If a short cervix is detected early:
Progesterone therapy may be given to reduce the risk of preterm birth.
A cervical cerclage (a stitch placed to close the cervix) may be performed in certain cases.
Activity modification or closer monitoring may be advised.
When and How It’s Measured
When: Typically between 16 and 24 weeks in high-risk pregnancies.
How: Using transvaginal ultrasound, which gives the most accurate measurement.
Conclusion
Monitoring cervical length is a key part of prenatal care for women at risk of preterm labor. Early detection of cervical shortening allows for interventions that can significantly improve pregnancy outcomes.